What to expect from chemotherapy treatment
Gonzalo
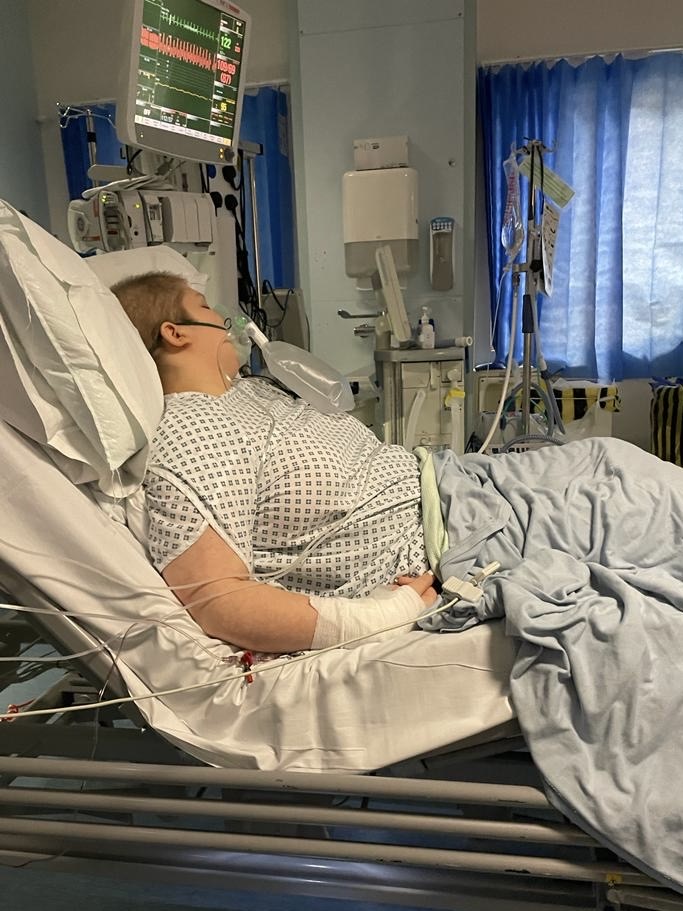
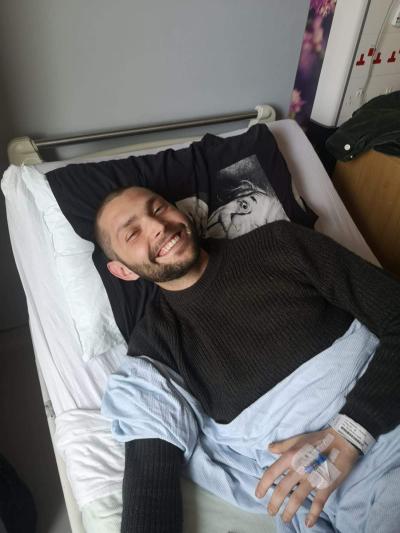
Gonzalo, who was diagnosed with Hodgkin lymphoma, shares his experience of chemotherapy sessions and offers some tips on how to cope with the visits.
My chemotherapy experience
I was diagnosed with stage 4 Hodgkin lymphoma in late 2021, aged 23. My treatment involved six rounds (12 sessions) of a chemotherapy combination called ABVD, which is used to treat Hodgkin lymphoma, spaced over six months. Since the cancer had spread into the lungs, it made radiotherapy very high risk.
How long does chemo take?
My chemotherapy involved a six hour visit to the hospital every two weeks. My first chemo session was both the most difficult and the easiest. The most difficult because I had no idea what to expect. Would it be painful, and would the side effects would be as bad as people said? In the end, it was actually the easiest as the side effects were the mildest I experienced.
What happens when you have chemo?
The side effects became more intense as the chemo sessions progressed. It was something I was told several times and expected, but only once I started living through it did I realise just how true that was, and how much I had to adapt my life as a result of it.
Chemo sessions would usually follow the same script. I’d go into the hospital, often feeling a headache and nausea building up as I got closer to the ward (I later found out that’s common in patients, and is called “anticipatory nausea”). After being warmly greeted by the Teenage Cancer Trust staff, I would get a new cannula with every session.
Cannulation was what worried me the most in the first few sessions. If the nurses struggled to get the cannula in on the first time, that would further add to my worry, which would worry the nurses even more, creating a chain of nervousness. For the first six sessions it took at least three painful attempts. I then learned to befriend the process of cannulation (I talk about how below), and since then the cannula started going in first-time.
Once the cannula was in, I’d get four different intravenous (IV) drugs, starting with a syringe filled with a bright red drug nicknamed “The Red Devil” by other cancer patients. I’d then have two different IV drugs which would take an hour each. The first one had to be stored in a fridge, making the experience of it entering my arm feel like my bones were slowly turning into ice. I found that using a heat pad on my arm really helped to ease the pain.
As the chemo sessions progressed, eating and drinking became more difficult due to a rising wave of nausea - I’d highly recommend avoiding foods and tastes you enjoy that day to keep your blacklist of food as short as possible.
Throughout this, I’d have some activities, conversations or music jams with the visitors that came with me, the Teenage Cancer Trust Youth Support Coordinator in the ward, and sometimes the nurses. This was a perfect distraction from my IV pole.
What is a chemo flush?
Once I’d had all the chemo, I’d get a “flush” of water through the cannula, get my collection of pills, and go home feeling the same nausea and fatigue that my clothes must feel when they’re taken out of the washing machine.
My chemo preparation checklist
1. Talk to other patients and staff
Talking to other patients while you’re in the ward is one of the easiest ways of getting the medicine of relatability. You’ll either get helpful tips for dealing with side effects, laugh at the absurdity of the situation, or connect with someone who understands and relates to what you’re going through.
Alternatively, talk to the nurses. It’ll make the process feel less cold and clinical, and you can also get some practical advice. With them, it’s often the case of “a problem shared is a problem halved.”
2. Take something into the session that will make it ‘enjoyable’
My chemo sessions completely changed when I started combining them with an enjoyable activity or taking something into the sessions with me. A couple of times, the visitors who came with me and I would take instruments and jam while I was getting chemo. I wouldn’t spend the few days leading up to it building up tension, but genuinely looking forward to the session.
3. Plan activities to distract yourself
After sharing with Nicola, the Teenage Cancer Trust Youth Support Coordinator, that my partner and I had been painting since the start of my treatment, she challenged us to make a painting with our feet. Accepting the challenge, Nicola got all the supplies, and in the next chemo session my partner and I went on to paint two full canvases using only our feet. The paintings looked like a combination of a canvas lathered with lasagne and what a five-year-old would paint when trying to symbolise freedom. It also completely distracted me from the robotic noises of the IV drip and the nausea that was building up. The painting is still in the ward, and I hope it stays there indefinitely. This is only one of multiple examples of activities we pre-planned to steer my focus away from the chemo and make the sessions more playful.
4. Befriend the process of cannulation
Of the 12 sessions of chemo I had, six of them were unnecessarily stressful from how nervous I was with the cannula, and six of them were much easier. In the first six sessions, I’d frequently leave with bruised arms and hands, as it would take on average three attempts to get the cannula in, and as many frustrated nurses. As my entire body was tensed up, it was more difficult for the nurses to either find good veins or keep the cannula in. Realising this was making the process more difficult for both them and myself, I tried a few methods to stop resisting it. One that really helped was the simple technique of focusing on my breathing, and making my exhales longer than my inhales, and with my eyes closed visualising what this would look like.
5. And remember that it’s medicine. Despite the downsides, it’s saving your life